Thin Uterine Lining: Causes, IVF Success Rates & Treatments
Being told you have a thin uterine lining can feel overwhelming—especially if you’re preparing for IVF or trying to conceive. The good news is that thin endometrium is often treatable, and many patients go on to achieve successful pregnancies with personalized care.
What Is the Uterine Lining?
The endometrium is the inner lining of the uterus where an embryo implants and grows. Each month, estrogen stimulates the lining to thicken in preparation for pregnancy. If pregnancy does not occur, the lining sheds during menstruation.
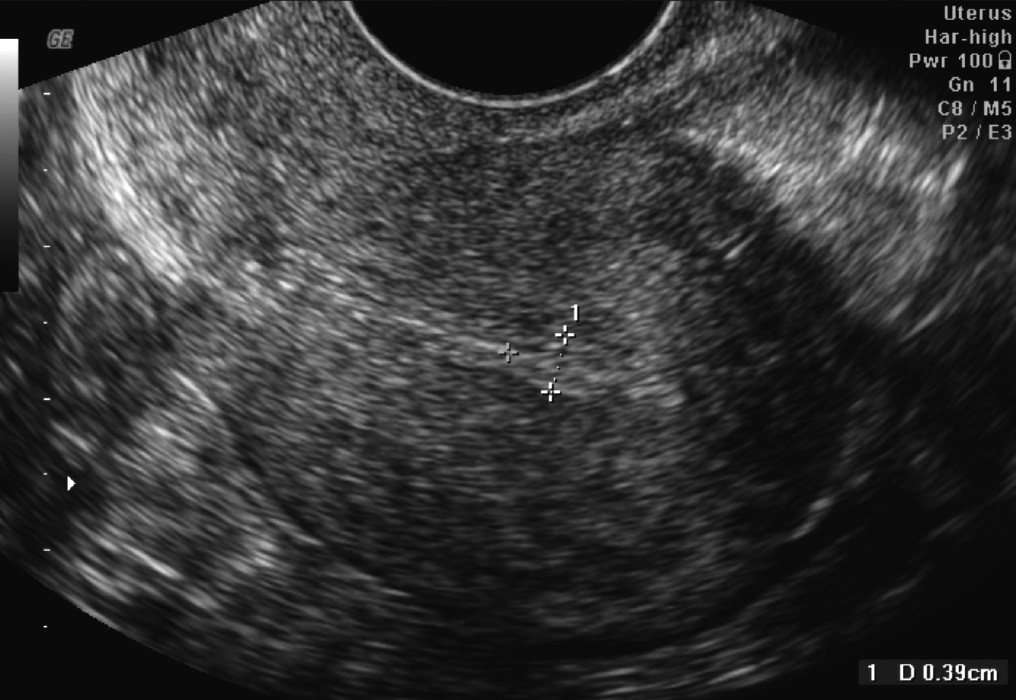
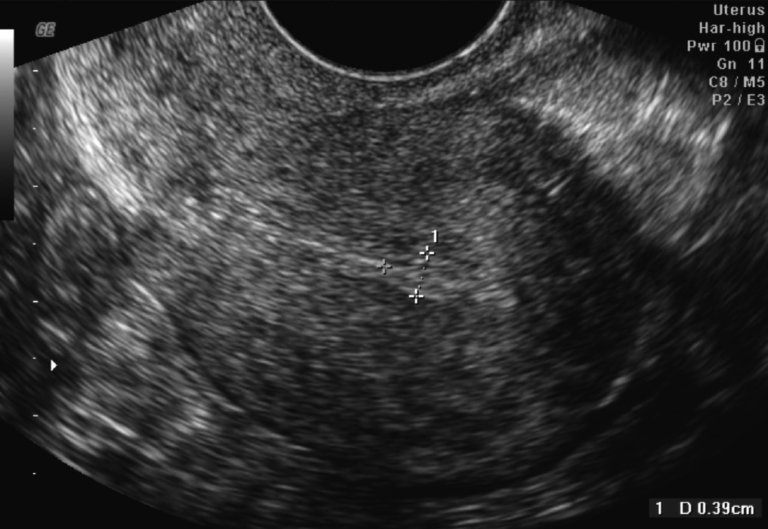
During fertility treatment, especially IVF, we measure endometrial thickness via ultrasound to determine whether the uterine environment is optimal for implantation.
How Thick Should the Uterine Lining Be for IVF?
While there is no single “perfect” number, many fertility specialists aim for a lining of approximately 7–12 mm before embryo transfer.
- 7–12 mm: Generally considered favorable
- Under 6–7 mm: May be associated with lower implantation rates
- Pattern and blood flow also play important roles
What Causes a Thin Uterine Lining?
Low Estrogen Levels
Estrogen drives endometrial growth. Low levels can prevent adequate thickening.
Uterine Scar Tissue (Asherman Syndrome)
Scar tissue from prior procedures such as D&C can interfere with normal lining development.
Poor Uterine Blood Flow
Reduced circulation may limit the endometrium’s ability to thicken properly.
Age-Related Hormonal Changes
Declining ovarian function may affect estrogen production and lining growth.
Can You Get Pregnant with a Thin Lining?
Yes. Pregnancy is still possible with a lining under 7 mm, though success rates may vary. Implantation depends on multiple factors including embryo quality, hormone timing, uterine cavity health, and lining pattern—not just thickness alone.
Treatment Options for Thin Endometrium
Estrogen Therapy
Oral, patch, or vaginal estrogen may stimulate lining growth during IVF or FET cycles.
Protocol Adjustments
Medication timing or dosing changes may improve endometrial response.
Hysteroscopy
If scar tissue is suspected, a minimally invasive hysteroscopy can diagnose and treat adhesions.
Targeted Supportive Therapies
In select cases, additional treatments may be considered to improve blood flow and endometrial receptivity.
When to See a Fertility Specialist
- Lining repeatedly measures under 7 mm
- IVF cycles have been canceled due to thin lining
- History of miscarriage with D&C
- Recurrent implantation failure
Caperton Fertility Institute provides individualized fertility care in Albuquerque, NM and El Paso, TX. If you are concerned about thin uterine lining, schedule a consultation to discuss personalized options.